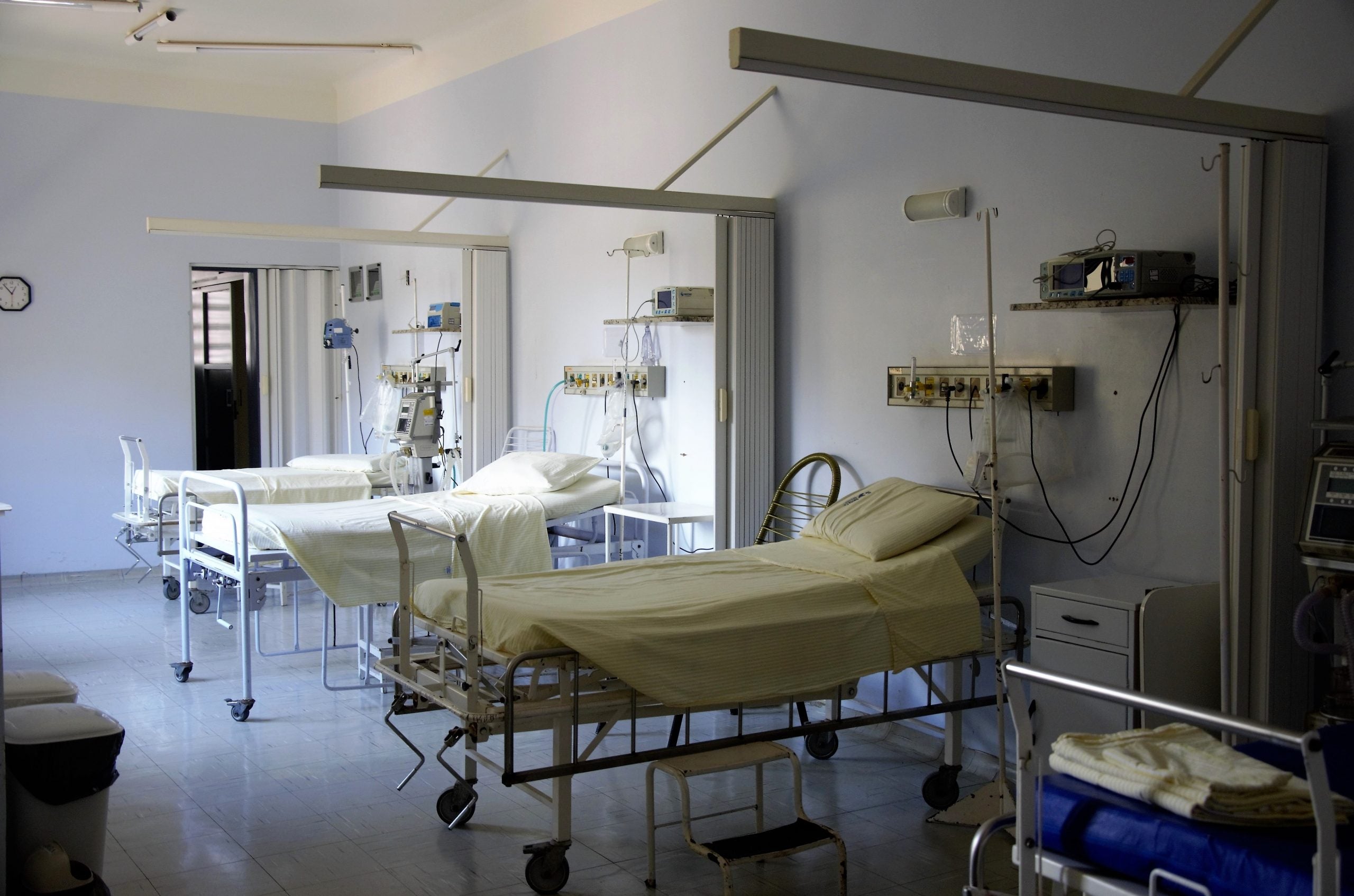
New research shows compelling disparity in critical care resources in the year preceding the COVID-19 pandemic
Specialized post-acute hospital beds were unavailable or inaccessible for many patients and providers across major cities and states.
Post-acute care, or the ongoing health care one receives after leaving a hospital, is largely unknown to many patients and their families. At the onset of the COVID-19 pandemic, some providers feared that there would be shortages of critical care resources, which includes the types of services that fall under the post-acute care umbrella , to adequately control the spread of infections and supply vital care to those infected.
A research team at the Health Care Financing Initiative (HCFI) at Georgetown’s McCourt School of Public Policy conducted a study of the long-term acute care hospitals in place before the pandemic began to better understand how available or unavailable post-acute care was for medically-complex patients.
“We started this exploration looking at the geography we felt we understood, so we looked close to home,” says Dr. Carol Davis, associate director of research and publications at HCFI. “The availability of specialized post-acute hospital beds varied quite significantly in the Mid-and South-Atlantic regions of the US.”
Key findings from the report on disparities in critical care capacity:1. There is a clear geographic disparity in access to and availability of post-acute hospital care. The barrier created by geographic distance is relevant from both a patient and provider perspective. Dr. Davis likens the importance of post-acute care facilities to fire departments. “They’re not needed 365 days a year, but they’re ready for action because when you need them, it is often life threatening.”
2. Specialized services that are infrequently needed might not be available everywhere, all the time. There are limits to providing these services everywhere, especially in rural areas. However, Dr. Davis says, “hospitals must maintain the ability to scale up as needed during urgent moments and leverage existing skills and expertise so that patients can still get the adequate care they need.”
3. In some places, there are no long-term acute care hospitals. Seventeen of the 56 hospital referral regions examined — across eight states plus the District of Columbia — have no long-term acute care hospitals. Patients who transfer to an alternate care setting often tie up critical staff at short-term hospitals. Travel to a distant long-term acute care hospital creates challenges for originating caregivers and family members coordinating or supporting a patient’s care.
4. Emergency and “what if” scenarios must be included in policy making around efficiency in health care spending. The research findings illustrate a need “for coverage and funding that aligns with expected volume and also allows for less predictable care to be served with temporary capacity increases when and where possible,” says Dr. Davis.
From a policy maker’s perspective, hyper-specialized care facilities can be difficult to justify, though Dr. Davis believes the health care system must maintain a certain level of readiness and expertise. “Some hospitals have invigorated conversations with post-acute hospital providers,” she says, “and are working to develop relationships and joint ventures to help existing facilities and providers meet the spikes in high-acuity patient care demands.”
The ongoing COVID-19 public health emergency highlights the need for broad coverage and availability of critical health resources. Even after the emergency subsides, post-acute hospital providers may be vital resources for understanding how to minimize and care for the long-term health effects seen in people exposed to COVID-19. “We’re still thinking about beds, capacity, resources and care-team relationships,” says Dr. Davis. “This will remain a pertinent topic that needs further research and analysis.”
Click here to read the full report and findings.
Dr. Carol Davis is an assistant research professor in the McCourt School of Public Policy and associate director of research and publications at the Health Care Financing Initiative. Her research focuses on public policies that govern access to health care and medical-financial security.
Dr. Thomas DeLeire is a professor in the McCourt School of Public Policy and director of the Health Care Financing Initiative. His research focuses on policies to improve health care access and outcomes, and on the dynamics between these policies and labor markets.
Teneil Brown is a programmer analyst at the Health Care Financing Initiative in the McCourt School of Public Policy. She specializes in analyzing and programming health care data using SAS and Stata.
Vidhur Krishna is a graduate research assistant at the Health Care Financing Initiative and a Master of Public Policy candidate in the McCourt School.
- Tagged
- Healthcare
- Research